Article Information:
-
Jamie Lamb
Vice President of Claims Operations -
Stacie Jenkins, RN, MSN, CPSO
Vice President, Patient Safety and Risk
Post Date:
01/25/2023
Article Categories:
- Medical Staff
- Patient Education
- Claims & Liability
- Patient Safety

How To Deal With Non-Compliant Patients
What happens when a physician sees a patient who does not follow medical advice or treatment instructions? How to deal with non-compliant patients is a vitally important skill — for the well-being of the patient first and foremost.
But, despite the best efforts of physicians, nurses, and other medical professionals, the non-compliant patient may choose to continue ignoring their advice — sometimes with catastrophic results. In those cases, proper documentation of the treatment plan and the patient’s refusal to apply it is important evidence should the patient decide to file a complaint against the physician.
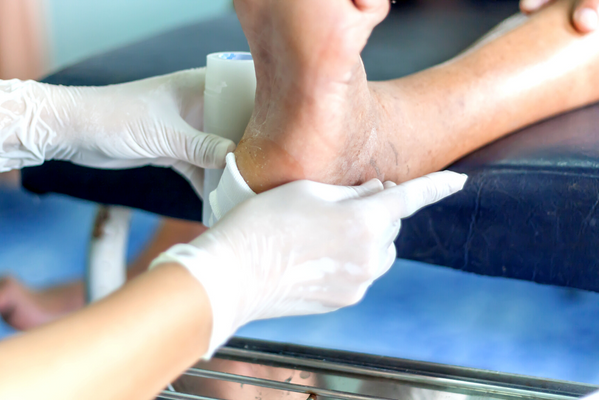
The Patient
A 72-year-old male patient was suffering from decubitus wounds on his foot and leg. The patient was also a smoker and a diabetic.
During his first visit to the physician, the wounds were debrided, and a topical antibiotic ointment was applied to the wound. The patient was also prescribed a special shoe to help with offloading the wounded foot. He was advised to quit smoking and schedule an appointment with a diabetic nutritionist to help him better treat his diabetes.
However, the patient continued to smoke against medical advice and did not schedule the recommended nutritionist appointment. The physician scheduled an appointment with an orthotic company to begin the process of manufacturing a shoe insert for the patient. The physician also ordered an arterial ultrasound, and the results came back normal.
The patient’s lack of healing progress and non-compliance with physician orders were documented in the chart along with wound photos.
The patient continued to see the physician on an almost weekly basis. A total contact cast (TCC) was placed on the patient to reduce pressure on the foot wound and promote healing. The TCC is often used on diabetic patients to help offload a foot with decubitus wounds.
The patient’s condition eventually worsened, and he had to undergo a below-the-knee amputation.
The Claim
The patient filed a PCF complaint against the physician, who claimed he treated the patient’s condition according to the standards of patient care for a foot wound in a diabetic patient.
According to his statement, the two biggest factors in the wounds not healing properly were the patient’s continued non-compliance through smoking and poorly controlled diabetes. These issues were mentioned to the patient during each visit and — equally important from a professional liability standpoint — the chart was regularly documented to reflect this communication.
The Medical Review Panel found no deviation from the standard of care. The panel noted that the doctor “followed all of the evidence-based recommendations for treatment of this condition. A proper workup was performed with appropriate therapy, surveillance, and follow-up appointments.”
When it comes to treating non-compliant patients, accurate documentation of non-compliance and physician suggestions in the chart at the time of an appointment can make the difference between a favorable or non-favorable legal outcome.
The Solution
Dealing with non-compliant patients is a day-to-day challenge for healthcare providers who have limited control over what their patients do in their daily lives. A patient relationship always places patient safety first, even in the case of non-compliant patients.
In the above case, the standard of care was found to be met. However, there are several approaches that may help a patient become more compliant.
Healthcare providers should consider these three additional factors to possibly identify barriers to compliance:
Patient Education
Has the patient been properly educated on the underlying medical condition and risks involved? Provide the patient with as many educational resources as possible regarding their condition and risks such as handouts, websites, and other resources. Make sure the patient understands their condition and the consequences rejecting medical advice could have on their overall health outlook.
Patient Disabilities and Resources
Does the patient have a hearing disability or a mental barrier? Does the patient have adequate insurance and/or financial resources to pay for the recommended treatment?
Have a social worker, case manager or risk manager meet with the patient to discuss discharge needs, current living environment, and any special needs the patient may have that are contributing to the non-compliance. If any opportunities are identified, the social worker/case manager can possibly provide external resources for the patient.
Patient Needs and Access
Is the patient uncomfortable or embarrassed by their current health conditions and/or lifestyle choices? Is the patient forgetful? Schedule appointments for the patient with recommended services. Even if the patient does not attend the scheduled appointment, an attempt was made to help the patient become more compliant.
In this particular case, the physician could have scheduled the patient an appointment with a diabetic nutritionist and a smoking cessation program. Both appointments would have provided more resources for the patient.
Going above and beyond the standard of care might be the key to getting a patient to become more compliant with the physician’s recommendations for treatment.
The Importance of Documentation in Healthcare
Good documentation practices are key to patient safety, accurate medical records, and ultimately, accountability for maintaining a proper standard of care within your physician’s practice.
Documentation should be objective, not subjective. Document facts and keep personal opinions out of the charting. While it might be tempting to allow an unpleasant opinion of a non-compliant patient to color the charting of their case, the nurse is telling the story of the patient. It should not include any personal judgment or bias.
Avoid general statements that can be misconstrued by others. Document the care provided to the patient clearly and in detail. Charting should be clear enough for someone to come back a year later and understand the entirety of the care provided based on what was documented.
It simply cannot be repeated enough — accurate, thorough documentation is a vital piece of defense that can help shield your practice from liability claims.
The Patient Relationship
The patient relationship can be complicated. It relies on good communication between physician and patient to work properly. Learning how to deal with non-compliant patients allows physicians to preserve their patient’s safety through education — helping them to better understand their conditions and heal based on a treatment plan.
In the worst-case scenario? Physicians then rely on proper documentation techniques to show they performed the accepted standard of care and did the best job possible to communicate with their patients. Ultimately, it is the patient’s choice to accept or disregard medical advice.
Looking for more information about why documentation matters in healthcare? Read this claim study.
About the Authors

Jamie Lamb
Director of Claims Operations, LHA Trust Funds
Jamie Lamb began her career in claims in 1997. Her experience includes handling multi-line claims in the areas of general liability, medical malpractice, automobile liability, commercial and personal property, excess and umbrella policies, and professional liability. Her experience comes as a former Manager and Litigation Specialist for the American National family of companies. She has been highly involved in the education and training of both internal and external customers her entire career. Ms. Lamb attended both Evangel University in Springfield, Missouri, and Loyola University in New Orleans.

Stacie Jenkins, RN, MSN, CPSO
Vice President of Patient Safety and Risk, LHA Trust Funds
Stacie Jenkins is a registered nurse with a master’s degree in nursing informatics. She has more than 20 years of experience in healthcare, working in patient care and quality/performance improvement positions. As the Vice President of Patient Safety & Risk at LHA Trust Funds, she works closely with hospital administrators, risk managers, and nursing staff to improve patient safety and establish best practices. She conducts on-site assessments and gives presentations designed to help clients address their patient safety risk management challenges.